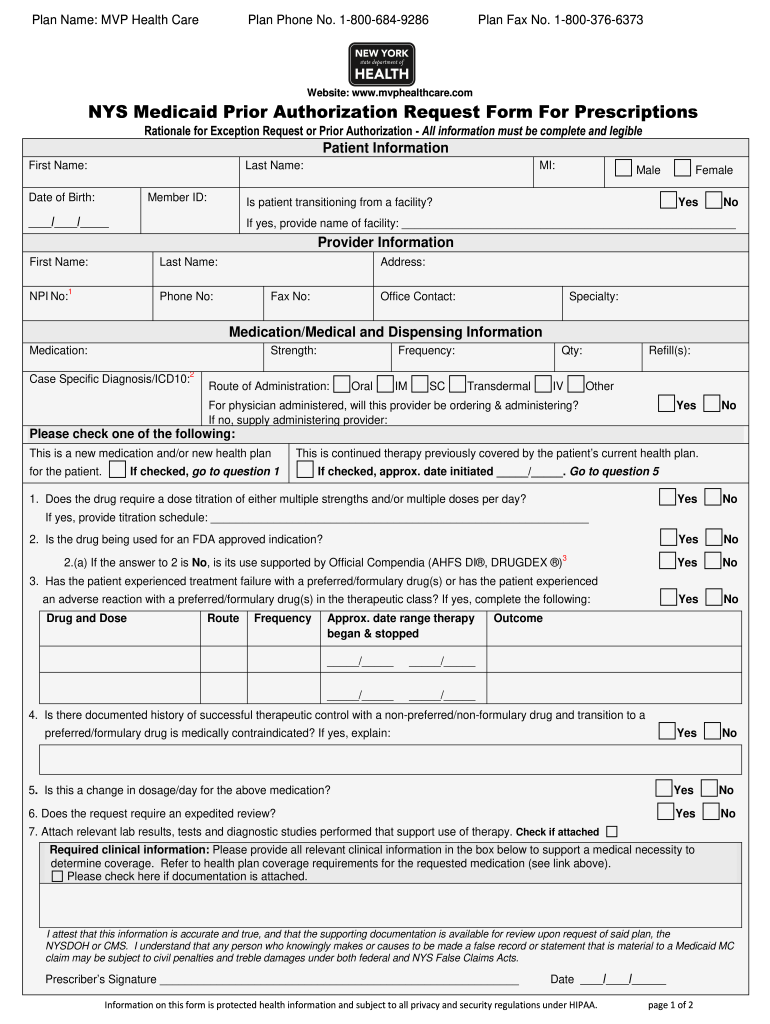
Caresource Prior Authorization Form
Caresource Prior Authorization Form - Easily fill out pdf blank, edit, and sign them. Web we want you to easily find the forms you need for your caresource plan. Your provider must get prior authorization before you get any of these services. Covermymeds automates the prior authorization (pa) process making it the fastest and easiest way to review, complete and track pa requests. Covermymeds is caresource prior authorization forms’s preferred method for receiving epa requests. Make use of the tools we offer to fill out your form. Save or instantly send your ready documents. Illegible or incomplete forms will be returned. They must also fall within the terms Web caresource prior authorization prior authorization (pa) is how we decide if the health services listed below will be covered by your caresource plan.
Web select the appropriate caresource form to get started. Web approved prior authorization payment is contingent upon the eligibility of the member at the time of service. Covermymeds is caresource prior authorization forms’s preferred method for receiving epa requests. Locate rad md prior auth imaging caresource and click on get form to get started. Web attach clinical notes with history and prior treatment. Illegible or incomplete forms will be returned. Prior authorization requests without medical justification or previous medications listed will be considered incomplete; Web caresource® evaluates prior authorization requests based on medical necessity, medical appropriateness and benefit limits. They must also fall within the terms Your provider must get prior authorization before you get any of these services.
Services billed must be within the provider’s scope of practice as determined by the applicable fee/payment schedule and the claim timely filing limits. Web select the appropriate caresource form to get started. Save or instantly send your ready documents. Web attach clinical notes with history and prior treatment. Make use of the tools we offer to fill out your form. Web caresource prior authorization prior authorization (pa) is how we decide if the health services listed below will be covered by your caresource plan. Prior authorization requests without medical justification or previous medications listed will be considered incomplete; Your provider must get prior authorization before you get any of these services. Illegible or incomplete forms will be returned. Covermymeds automates the prior authorization (pa) process making it the fastest and easiest way to review, complete and track pa requests.
Bcbs Prior Authorization Form Michigan Form Resume Examples kDp3Og030Q
Web attach clinical notes with history and prior treatment. Web caresource prior authorization prior authorization (pa) is how we decide if the health services listed below will be covered by your caresource plan. Web caresource® evaluates prior authorization requests based on medical necessity, medical appropriateness and benefit limits. Make use of the tools we offer to fill out your form..
Work From Home Prior Authorization Jobs — Intake Agent Prior
Covermymeds automates the prior authorization (pa) process making it the fastest and easiest way to review, complete and track pa requests. Covermymeds is caresource prior authorization forms’s preferred method for receiving epa requests. Web select the appropriate caresource form to get started. Web the best way to modify and esign caresource imaging prior authorization form without breaking a sweat. Easily.
Sample Caremark Prior Authorization Form 8+ Free Documents in PDF
Locate rad md prior auth imaging caresource and click on get form to get started. Covermymeds is caresource prior authorization forms’s preferred method for receiving epa requests. Save or instantly send your ready documents. Web caresource® evaluates prior authorization requests based on medical necessity, medical appropriateness and benefit limits. Web caresource prior authorization prior authorization (pa) is how we decide.
Prior Authorization Form Priorityhealth Download Fillable PDF
Services billed must be within the provider’s scope of practice as determined by the applicable fee/payment schedule and the claim timely filing limits. Web attach clinical notes with history and prior treatment. They must also fall within the terms Locate rad md prior auth imaging caresource and click on get form to get started. Save or instantly send your ready.
Fillable Kentucky Medicaid Mco Prior Authorization Request Form
Web the best way to modify and esign caresource imaging prior authorization form without breaking a sweat. Your provider must get prior authorization before you get any of these services. Listed below are all the forms you may need as a caresource member. Illegible or incomplete forms will be returned. Web approved prior authorization payment is contingent upon the eligibility.
Fillable Indiana Health Coverage Programs Prior Authorization Request
Illegible or incomplete forms will be returned. They must also fall within the terms Web the best way to modify and esign caresource imaging prior authorization form without breaking a sweat. Locate rad md prior auth imaging caresource and click on get form to get started. Web caresource® evaluates prior authorization requests based on medical necessity, medical appropriateness and benefit.
Pharmacy Prior Authorization Form Sample Templates
Web the best way to modify and esign caresource imaging prior authorization form without breaking a sweat. Prior authorization requests without medical justification or previous medications listed will be considered incomplete; Covermymeds automates the prior authorization (pa) process making it the fastest and easiest way to review, complete and track pa requests. Web caresource® evaluates prior authorization requests based on.
Caremore Prior Authorization Form Fill Out and Sign Printable PDF
Listed below are all the forms you may need as a caresource member. Illegible or incomplete forms will be returned. Easily fill out pdf blank, edit, and sign them. Save or instantly send your ready documents. Covermymeds is caresource prior authorization forms’s preferred method for receiving epa requests.
Prior Authorization Request Form printable pdf download
Web caresource prior authorization prior authorization (pa) is how we decide if the health services listed below will be covered by your caresource plan. Illegible or incomplete forms will be returned. They must also fall within the terms Locate rad md prior auth imaging caresource and click on get form to get started. Services billed must be within the provider’s.
Fillable Online Ohio Provider Medical Prior Authorization Request Form
Your provider must get prior authorization before you get any of these services. Illegible or incomplete forms will be returned. Web caresource prior authorization prior authorization (pa) is how we decide if the health services listed below will be covered by your caresource plan. Easily fill out pdf blank, edit, and sign them. Covermymeds automates the prior authorization (pa) process.
Web Caresource Prior Authorization Prior Authorization (Pa) Is How We Decide If The Health Services Listed Below Will Be Covered By Your Caresource Plan.
Web attach clinical notes with history and prior treatment. Easily fill out pdf blank, edit, and sign them. Web caresource® evaluates prior authorization requests based on medical necessity, medical appropriateness and benefit limits. Save or instantly send your ready documents.
Illegible Or Incomplete Forms Will Be Returned.
Web approved prior authorization payment is contingent upon the eligibility of the member at the time of service. They must also fall within the terms Services billed must be within the provider’s scope of practice as determined by the applicable fee/payment schedule and the claim timely filing limits. Listed below are all the forms you may need as a caresource member.
To See The Full List Of Forms For Your Plan, Please Select Your Plan From The Drop Down List Above.
Covermymeds is caresource prior authorization forms’s preferred method for receiving epa requests. Web we want you to easily find the forms you need for your caresource plan. Make use of the tools we offer to fill out your form. Covermymeds automates the prior authorization (pa) process making it the fastest and easiest way to review, complete and track pa requests.
Prior Authorization Requests Without Medical Justification Or Previous Medications Listed Will Be Considered Incomplete;
Web select the appropriate caresource form to get started. Web the best way to modify and esign caresource imaging prior authorization form without breaking a sweat. Locate rad md prior auth imaging caresource and click on get form to get started. Your provider must get prior authorization before you get any of these services.